Escherichia coli (E. coli)
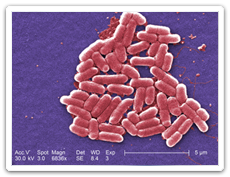 Escherichia coli (called E. coli) is a bacterium that is commonly found in the intestinal tract of animals and humans. Most types of E. coli will not make a person sick,
but some can cause mild to severe illness.
Escherichia coli (called E. coli) is a bacterium that is commonly found in the intestinal tract of animals and humans. Most types of E. coli will not make a person sick,
but some can cause mild to severe illness.
Shiga toxin-producing E. coli (STEC)
Shiga toxin producing E. coli (STEC) is also referred to as verocytotoxin-producing E. coli (VTEC) or enterohemorrhagic E. coli (EHEC). These are strains of the E. coli bacteria that cause illness by making a toxin called Shiga toxin. They are often associated with foodborne outbreaks and are more likely to cause severe illness than other types of non-Shiga toxin-producing E. coli.
The most commonly identified STEC bacteria is E. coli O157:H7, but other non-O157 STEC E. coli can also cause illness.
Public Health Notices and Food Recall Warnings
The following links provide information for Public Health Agency of Canada (PHAC) public health notices related to active E. coli outbreaks occurring in Canada. These notices are to inform Manitobans of the potential risk for exposure to E. coli due to consumption of these food items which may have been distributed within Manitoba or are available to order online. Further information on food recall notifications and warnings specific to each outbreak is listed within each notice.
- There are currently no active E.coli outbreaks occurring in Canada.
Symptoms
Symptoms of STEC infection generally appear three to four days after a person becomes infected but can range from the day the exposure occurred, and up to 10 days after. STEC infection can vary in individuals but often includes watery diarrhea, vomiting, and stomach cramps. In severe cases, diarrhea may become bloody and other symptoms such as a high fever can occur.
Most people recover within seven to 10 days, but the bacteria can continue to be found in their stool for several days to weeks.
A small number (5 -10%) of individuals may develop a potentially life-threatening complication called hemolytic uremic syndrome (HUS), that affects the kidneys and blood clotting functions of infected people. Early signs of HUS can include decreased frequency in urination, extreme tiredness, and pallor (i.e., paleness of skin in the face). Treatment for HUS involves hospitalization, and may include blood transfusions, and kidney dialysis. Most people recover completely from HUS, but in some cases, it can be fatal.
An individual should consult a health care provider if any of the following moderate to severe symptoms develop:
- diarrhea that lasts more than 3 days;
- blood in the stool;
- high fever (102°F/ 38.9°C or higher);
- vomiting that is preventing them from drinking fluids;
- or decreased urination.
Causes
STEC bacteria naturally live in the intestines and feces (poop) of many animals, especially farm animals (e.g., cows, goats, sheep) and deer.
STEC infection is most often caused by eating food or drinking products contaminated with STEC bacteria such as:
- raw or undercooked hamburger or beef;
- raw produce, such as leafy greens like lettuce, sprouts, and spinach that has been contaminated with animal or human feces;
- unpasteurized (raw) milk, juices, and cider (e.g., apple cider);
- raw flour (e.g., cookie dough, cake batter);
- drinking water that has been contaminated with animal or human feces.
Other ways that individuals can be exposed to STEC bacteria include:
- fecal-oral (hand to mouth) contact with an animal, animal feces (poop), or environments where the animals live (e.g., agricultural fairs, petting zoos, farm visits);
- swimming in or swallowing contaminated water, such as in a lake contaminated by animal feces;
- touching or having direct contact with a person infected with STEC, and then touching the eyes, nose, or mouth (i.e., after changing the diaper of someone infected with STEC or helping someone with STEC use the toilet).
Improper hand hygiene and food handling contribute to the spread of illness.
Risk Factors
STEC infections can affect persons of all ages. Those at greater risk of developing severe illness are young children (less than 5 years old), older adults (aged 60 and older) and those with a weakened immune system.
Treatment
Drinking lots of fluids (i.e., water or clear fluids that are not high in sugar) is important to stay hydrated. Antibiotics and anti-diarrheal medications are not recommended. Antibiotics have no proven benefit and may cause harm by increasing the risk of developing HUS. Antidiarrheal products may also increase the risk of developing HUS by decreasing the body’s ability to eliminate the STEC bacteria which is shed in the stool.
For those that develop HUS, treatment involves hospitalization, and may include blood transfusions, and kidney dialysis.
Prevention
STEC infection can be prevented by:
- handwashing with soap and water after using the toilet, handling diapers, cleaning up after pets, contact with livestock and their environment, and before eating or preparing food. If soap and water are not available for handwashing, clean hands with an alcohol-based hand sanitizer;
- washing fruits and vegetables before preparation or eating;
- cooking ground beef thoroughly to an internal temperature of 71°C or until the juices run clear and the meat is no longer pink;
- drinking only pasteurized milk, juices, or cider;
- keeping raw meats separate from other foods during storage and preparation. Clean counters, and equipment (e.g., cutting boards, utensils) after contact with raw meat. Store raw meats in a refrigerator in separate containers that are sealed to avoid leaking onto other foods and surfaces;
- drinking water from sources that have been chlorinated, or boiled if the safety of the water is unknown;
- avoiding ingestion of water from streams, lakes, or swimming pools.
If you or your child develop symptoms of diarrhea:
- ensure thorough hygiene measures after using the toilet by handwashing with soap and water along with frequent cleaning and disinfection of washroom facilities used. If soap and water are not available for handwashing, clean hands with an alcohol-based hand sanitizer;
- place soiled diapers in a leak proof plastic bag prior to disposal;
- avoid preparing or handling food for others;
- limit direct contact with high-risk individuals (e.g., young children, older adults and those with a weakened immune system);
- avoid use of pools, hot tubs, and other recreational waters;
- If employed as a food handler, health care worker or childcare worker, you should report your symptoms to your manager. You should not be attending work. If you must attend work, you should be assigned to other duties that do no involve handling food or providing direct care to others until symptoms have resolved. Follow up with a health care provider is recommended if symptoms are moderate to severe. If you test positive for STEC infection, additional testing may be required as directed by Public Health before you return to work.
- Children that attend a childcare facility should stay home until 24-48 hours after symptoms have resolved. Follow up with a health care provider is recommended if symptoms are moderate to severe. If they test positive for STEC infection they will require additional testing before they can return to the childcare facility as directed by Public Health.
Manitoba Health Resources
For Health Care Providers
- Shiga Toxin-Producing Escherichia coli (STEC) Infection Protocol
September 2024 NEW
Other Resources
- Health Canada - Escherichia coli
- Centers for Disease Control and Prevention - Escherichia coli
- World Health Organization - E.coli
Communicable Disease
Control (CDC) Health Links – Info Santé |


